Although the term “vaccine hesitancy” has gained momentum in recent months, it fails to capture the systemic nature of the greater problem of vaccine access and lack of trust in public health institutions, especially among groups and communities that historically have been underserved and mistreated or even abused by the public health and medical care systems. We should rephrase it to “vaccine equity.”
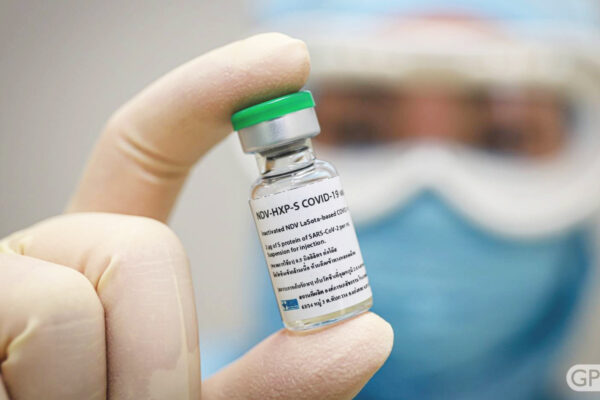
The COVID-19 pandemic undeniably hit communities of color the hardest. Disparities in testing, infection rates, rates of hospitalization and death in communities of color have been well-documented since the onset of the pandemic. And yet, according to the latest data available, the rate of vaccination within these groups lags well behind that of white individuals nationally, and Texas is no exception.
The initial rush for the vaccine is over. The Americans who now remain to be vaccinated are not the ones who were so eager they waited in hours-long lines to get the first shot, or so available that they could show up for any appointment time. The populations we must now try to reach are those who may be on the wrong side of the digital divide, those who are vulnerable to misinformation, those with limited transportation access, and those whose trust in public health institutions has eroded after centuries of structural racism.
By opting instead for the phrase “vaccine equity,” we reframe the issue in a critical way.
As tempting as it is to focus on stubborn or ignorant individuals, the real problem is twofold. First, we have a health care system that fails to engender trust. Second, the frenzied circumstances of the pandemic have led many to the unfortunate (and wrong) conclusion that listening to people is a luxury they can’t afford.
Another way is possible. We have an opportunity to design solutions that meet people where they are. The solutions that are working are the ones that recognize the disparities that exist and innovate ways to break down those barriers. Mobile vaccination sites, outreach through local churches, and other grassroots, community-based efforts are among the most effective ways we have seen of helping people overcome their issues of access and trust.
Mount Pleasant in the northeastern part of our state near Texarkana illustrates what we can do once we make mobilizing community resources the main focus. Residents of this town of 16,000 were not the most receptive to vaccination — at more than 40% Hispanic, with many undocumented, fear and mistrust of government was a barrier to vaccine acceptance.
Their experience holds many lessons. The town had enough of a critical mass of community members — faith leaders, health care workers and local organizations — who knew better than to write off their own community or treat hesitancy as an inalterable trait. By relying on trusted messengers, word-of-mouth and a willingness to meet people where they were, Mount Pleasant doubled its vaccination rate by early May, achieving this turnaround while vaccination rates slowed for the state as a whole.
This could be applicable across Texas, particularly in rural communities. This can happen only if public health experts are guided by more generous assumptions about those many have written off as “hesitant”: that if vaccines are ubiquitous, convenient, accessible and promoted by trusted voices in the community, for even more conservative areas it won’t be a question of if they get vaccinated, but when and how.
Systemic change is never simple, but we can start by calling things as they are. Not only is it inaccurate to talk about vaccine hesitancy at this stage in the pandemic — it sidesteps and ignores the reality of the situation. Vaccine access and trust are issues of equity, not hesitancy. The next chapter in America’s efforts to vaccinate its population depends on our understanding that distinction.
Octavio N. Martinez Jr. is the executive director of the Hogg Foundation for Mental Health at The University of Texas at Austin.
A version of this op-ed appeared in the Houston Chronicle, Austin American-Statesman, Waco Tribune Herald and the Lubbock Avalanche-Journal.